In a surgical first for St. Louis Children’s Hospital, Division Chief of Pediatric Otolaryngology David Leonard, MD, and a multidisciplinary team of surgeons repaired a rare birth defect and put a young patient back on a path to a normal life.
When Hiep Nguyen entered her local Wichita hospital in May 2020, she expected to give birth to a third child that would join two healthy brothers at home. But shortly after birth, as she held newborn Vincent in her arms, his heart rate dropped suddenly and he lost oxygen.

Doctors and nurses rushed to stabilize the infant, but the cause of his sudden change would not be known for another five days, when he was diagnosed with Laryngotracheoesophageal cleft Type 4 or Type 4 LTEC.
Type 4 is the most severe type of laryngeal cleft, an extremely rare congenital defect in which the airway passage and food passage do not separate correctly during development. Vincent’s secretions, instead of being swallowed, were going to his lungs, causing pain and tremendous difficulty breathing.
Sometimes it takes a village
The medical team in Wichita was not equipped to handle Vincent’s condition, which would require surgery soon if he was to survive. They explained to Hiep and her husband Eric that St. Louis Children’s Hospital was their best choice for care. It was there they met pediatric otolaryngologist, David Leonard, MD, and Martin Keller, MD, director of trauma at St. Louis Children’s Hospital.
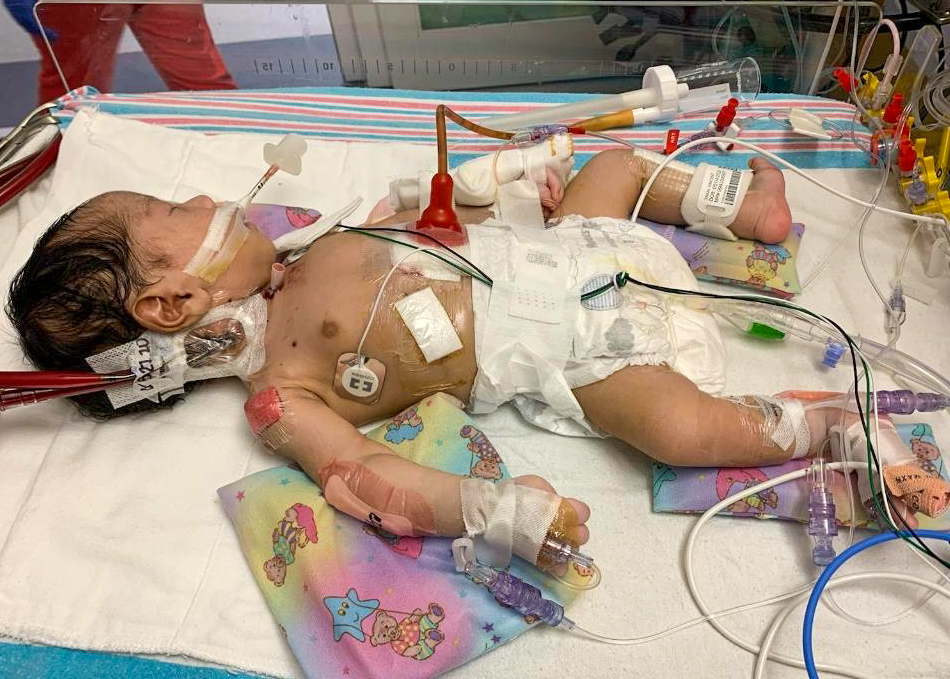
Scared for their newborn son and nervous about the rarity of his condition, Hiep’s first instinct was to ensure they had come to the right place.
“The first question I asked Dr. Leonard was if he had done this procedure before,” said Hiep. “His answer was no, but he proceeded to explain how Vincent’s presentation was a perfect fit for the team at Washington University and St. Louis Children’s Hospital. I was impressed by his honesty and straightforward approach and knew right then we were going to receive the care we needed.”
For another two weeks Vincent underwent a series of tests to confirm his diagnosis. The surgery lasted more than 10 hours and involved three pediatric surgical specialties – otolaryngology, general surgery and orthopedic surgery. Although the procedure was deemed successful, Vincent would experience a couple of frightening complications in the hours following.

Slow and steady road to recovery
The first night after surgery saw the first code blue – a blocked breathing tube that required Leonard and the entire NICU team to resolve successfully. Two days later Vincent experienced internal bleeding in his abdomen, which would require blood transfusions. Once again, a talented team of caregivers was able to stop the bleeding.
Vincent and Hiep would stay at St. Louis Children’s Hospital for nine months as the team of caring professionals advanced him through the stages of his recovery.
Today, he is home and in May will celebrate his third birthday. Vincent still uses a tracheostomy for breathing and a G-tube to eat, but he has recently started to be weaned from ventilator-assisted breathing. For the past several weeks he has been removed from the ventilator, initially for 30 minutes, twice each day, and currently for an hour. It is during these periods that he most enjoys going for walks and playing with his older brothers. He also enjoys his daily arts and crafts activities.
His care is continuous and requires full day in-home nursing care, with mom filling in on the weekends. Her training is another success she attributes to the remarkable team at WashU. Vincent hasn’t needed supplemental oxygen in over a year, so the family is hopeful he will one day be successfully decannulated (have his breathing tube removed) and lead a more active childhood.

Leonard is cautiously optimistic about Vincent’s progress.
“Vincent’s surgery was complicated and required a multidisciplinary effort, but it was just the beginning of his journey,” he explained. “Progress has been slow but steady, and now that he is starting to wean from his ventilator, there is real optimism that we will be able to decannulate him, although it may take 6-12 months to get him to that stage.”
According to Leonard, Vincent has also done incredibly well from a neurodevelopmental standpoint. He has an attentive, loving and supportive family who have helped him overcome his challenging start to life and reach his maximum potential. Everyone is hopeful that once he’s off his ventilator and decannulated that he will lead an essentially normal life.
