Washington University cancer scientists, led by Head and Neck Surgery Division Chief Sid Puram, MD, PhD, are using single cell genetic analysis to better understand the complexities of head and neck cancer and improve personalized medicine.
Personalized medicine is an emerging practice of medicine that uses an individual’s unique genetic profile to help guide prevention, diagnosis, and treatment of disease. A patient’s profile can help doctors select appropriate medical therapy and administer it using the proper dose or regimen.

Puram and his lab used single-cell RNA sequencing techniques to uncover a high level of cellular diversity both within and between patient tumor samples. Their prior work emphasized the role of such diversity in harmful cancer processes such as invasion and metastasis. The current work, published in the April 2023 issue of Nature Genetics, suggests tumor heterogeneity must also be considered during diagnosis and treatment of HPV-positive tumors.
Human papillomavirus, or HPV, is the most common sexually transmitted infection in the United States. It is the cause of more than 5% of all cancers worldwide, including all cervical cancers and most oropharyngeal squamous cell carcinomas (OPSCC).
Puram’s team conducted genetic profiling of cells from both HPV-negative and HPV-positive OPSCC to better understand differences in cancer severity, metastasis and patient survival. Overall, more than 70,000 cells were analyzed from 16 primary, untreated tumor samples—12 HPV-positive and four HPV-negative. A number of surprising observations were made that may help to guide future treatment paradigms:
- Several different cell types define the cellular diversity of any given tumor, the majority are malignant cells, but some are normal. Surprisingly HPV-positive tumors demonstrated an enriched population of cells in a senescent-like state, compared to HPV-negative tumors.
- The abundance and expression of a variety of HPV genes (E1, E2 and E4-E7) varies within and between HPV-positive tumor samples.
- Malignant cells were found in histologically-defined negative margins or the supposed normal tissue surrounding a tumor, possibly explaining tumor recurrence when surgically clear margins have been reported.
- HPV-positive tumors may include cells of unique states where HPV genes have been reduced or turned off, which may support observed diversity in resistance to treatment and explain why some HPV-positive tumors have good outcomes while others have bad outcomes.
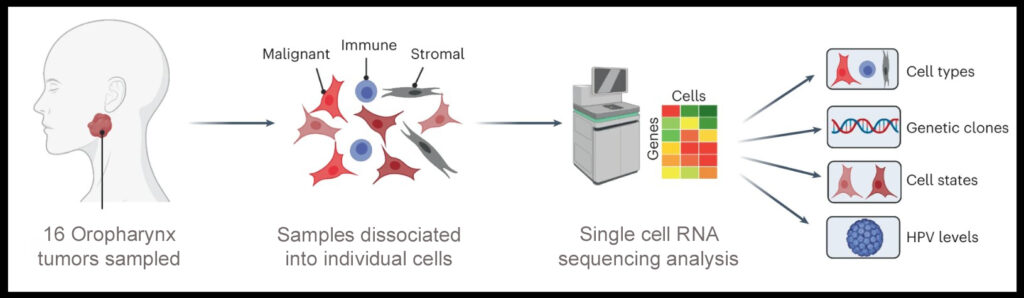
The study demonstrates the previously unappreciated diversity in genetic profiles and HPV gene expression found within individual OPSCC tumors and the important observation of invasive malignant cells in tumor-adjacent areas previously thought to represent clear surgical margins.
HPV-positive cells respond better to cancer treatments, possibly due to their enhance cell cycle activity. If a subset of these cells represses their HPV gene expression, they could become less susceptible to radiation and chemotherapy, then subsequently turn HPV expression back on, leading to tumor recurrence. These observations will guide important new considerations for treatment of HPV-positive OPSCC.
For more information about this study, please contact Sid Puram, MD, PhD.
