Amber U. Luong, MD, PhD, was three years old when she and her family fled Vietnam by boat. It was April 29, 1975, the day before the South Vietnamese capital of Saigon fell to the North Vietnamese Army.
The fact that she and her family were among the hundreds of thousands of boat people who survived the difficult passage, eventually making their way to the U.S., is not something she frequently discusses. As professor and vice chair of Research of Otorhinolaryngology at McGovern Medical School at the University of Texas Health Science Center at Houston, Luong will more likely share her enthusiasm for academic medicine, and her research on new treatments for chronic rhinosinusitis with polyps.
She is also likely to mention the importance of a supportive family network. As the mother of three busy children who are not old enough to drive, she is grateful to have family nearby to help. She might mention, with a smile, that her real job title should be “a surgeon-scientist by day and Uber driver by night.”

Having arrived in the U.S. as an immigrant, and the fact that she is one of the highest- ranking women in academic Otolaryngology today, are indelibly linked. So, in a rare occurrence, Luong will discuss her research as well as her background and its influence on her career, at the upcoming Ogura Lectureship and Resident Research Day on June 24.
Luong, who also has a joint appointment within the Center of Immunology and Autoimmune Diseases at the Institute of Molecular Medicine at UTHealth Houston, will present:
Revisiting the role of Fungi in CRS: Lessons learned from allergic fungal rhinosinusitis, and
An immigrant’s story on forging a rewarding career
In advance of her lecture, Luong shares her passion for academic medicine.
Register to attend Luong’s lecture virtually »
Why did you go into medicine?
When we came over here, my parents emphasized the importance of education. Because of the war, kids in Vietnam weren’t going to school anymore. My dad was a lawyer, and both my parents came from pretty affluent families. They said the only way to get out of a situation, after coming here and having no resources, was through education.
I took that to heart and kept going. I got my MD, PhD, got enrolled in a masters for science for clinical research, participated in the leadership of academic medicine to learn how to be a leader. Coming from my background, I am always looking for opportunities to learn. These opportunities are not always available to people throughout the world. It’s been quite a luxury so I’ve been soaking it up.
Why Otolaryngology?
I have a unique background, starting with my MD PhD training with the medical scientists training program at UT Southwestern in molecular genetics. At the same time I like surgery. At the time I was interviewing for residency programs, otolaryngology was perfect for combining those two interests. Ultimately, I discovered rhinology and the surgery we can do inside the nose, as well as the tissue we can study, and the patients with chronic disease we can follow.
Why is this an exciting time for students to go into medicine? And what guidance do you give medical students as they consider residency programs?
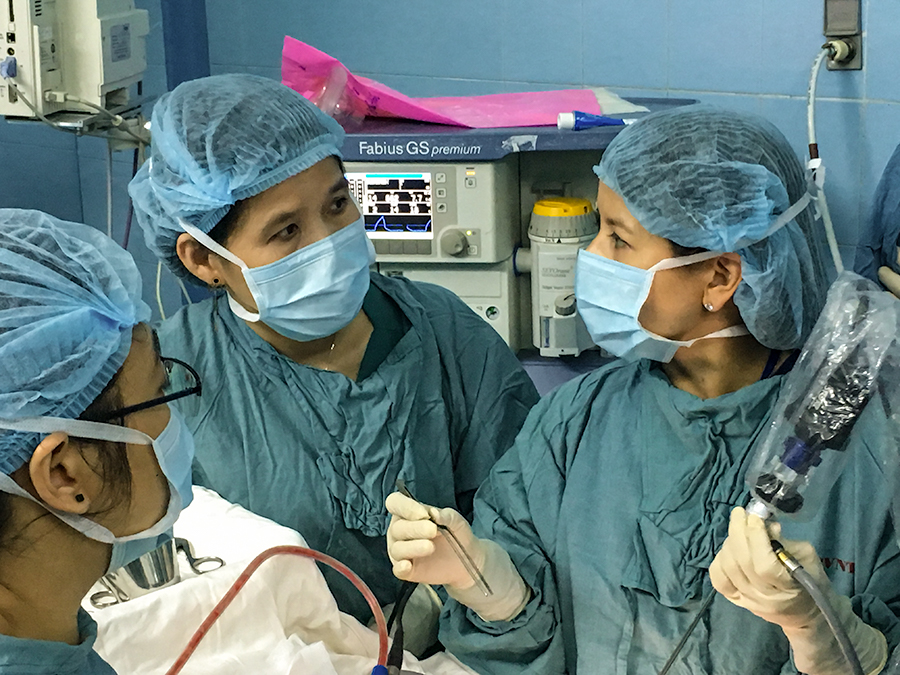
Although there are so many career opportunities out there, it is such an exciting time to go into medicine, especially otolaryngology. There has been a recent infusion of research and technology into the field such as robotics surgery, new means of localizing tumor cells, virtual reality incorporated with navigation and machine learning for identifying tumor attachment sites.
For those considering residency programs, luckily most ENT programs will train you well to be a surgeon. If I was looking into a program these days, I would not overlook the research program. Understanding how to do research is a key aspect of training that a lot of medical students don’t appreciate. Even if you go into private practice in a small town, it is critical to be able to pick up a journal to stay abreast of the field. However, you really need to understand how to critically evaluate studies to determine if this technique/understanding is something you should offer your patients. One should be able to understand the limitations of a study, and the only way you can do that is if you personally do research during your training. Even for those programs with shorter dedicated research months, you should look for structure in the program.
